Unlock the power of AI in clinical decision making
ClinicalKey AI combines trusted, evidence-based clinical content with conversational search powered by generative AI to support clinicians in delivering high-quality patient care

Unfortunately we don't fully support your browser. If you have the option to, please upgrade to a newer version or use Mozilla Firefox, Microsoft Edge, Google Chrome, or Safari 14 or newer. If you are unable to, and need support, please send us your feedback.
We'd appreciate your feedback.Tell us what you think! opens in new tab/window
Turn information into actionable knowledge to help healthcare professionals put evidence into practice.
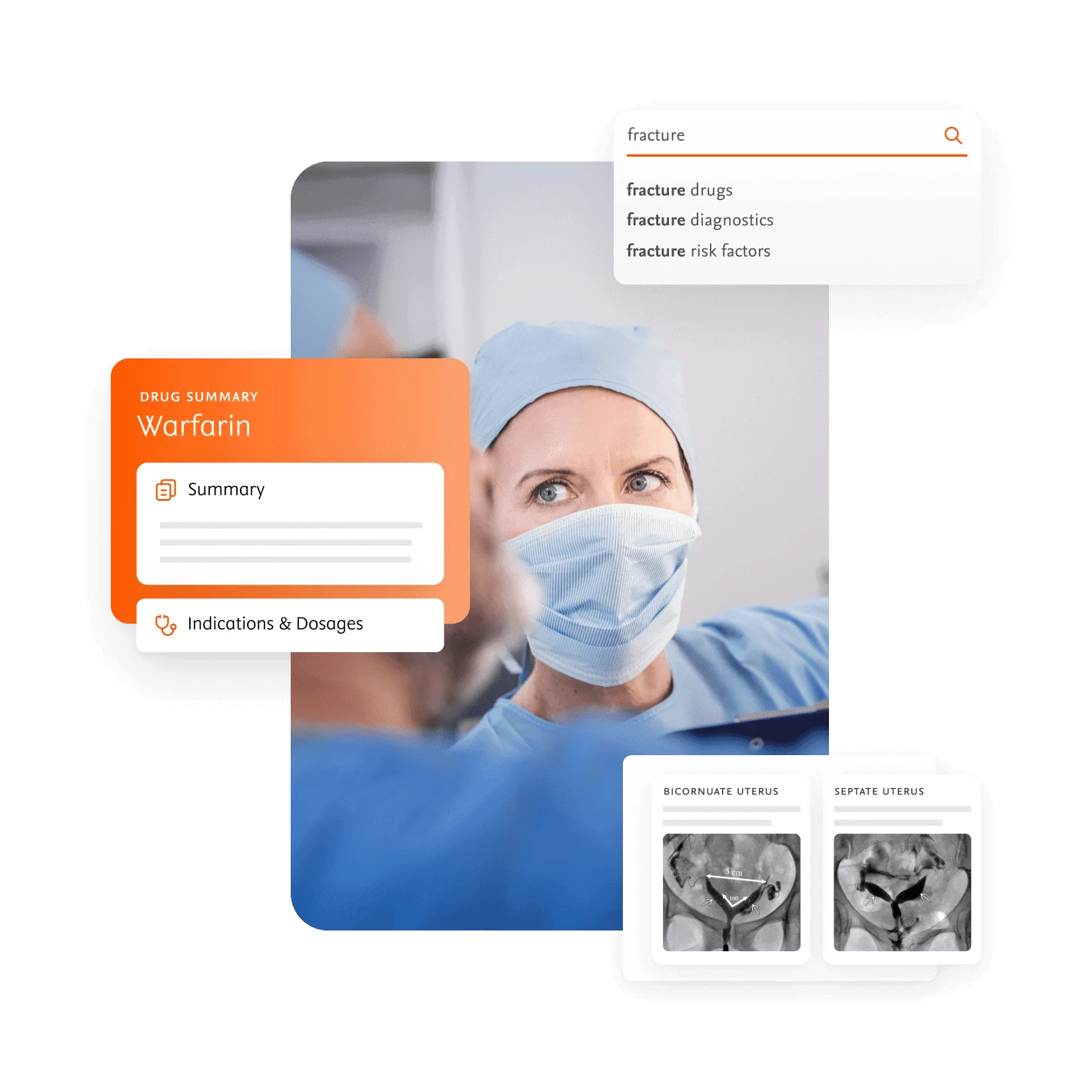
ClinicalKey AI combines trusted, evidence-based clinical content with conversational search powered by generative AI to support clinicians in delivering high-quality patient care

ClinicalKey enables clinicians to stay abreast of rapidly expanding clinical knowledge

ClinicalPath provides evidence-based oncology pathways embedded in the clinical workflow, helping teams make consistent, well-informed decisions for high-quality care
Order Sets enables organizations to author, review and manage order sets in a collaborative environment

Integrate Gold Standard Drug Database and clinical decision support into your workflow
Clinical Pharmacology powered by ClinicalKey empowers pharmacists to guide optimal drug treatment

Clinical Skills allows clinicians to access skills and procedures in the EHR and at bedside to support daily patient care
ClinicalKey for Nursing empowers clinicians with actionable answers to efficiently carry out treatment plans
Care Planning combines the patient’s story, evidence-based care plan guides, and standardized assessments into one longitudinal plan of care

STATdx helps radiologists make informed and efficient decisions with direct access to trusted information
ExpertPath gives pathologists tools to make confident diagnoses
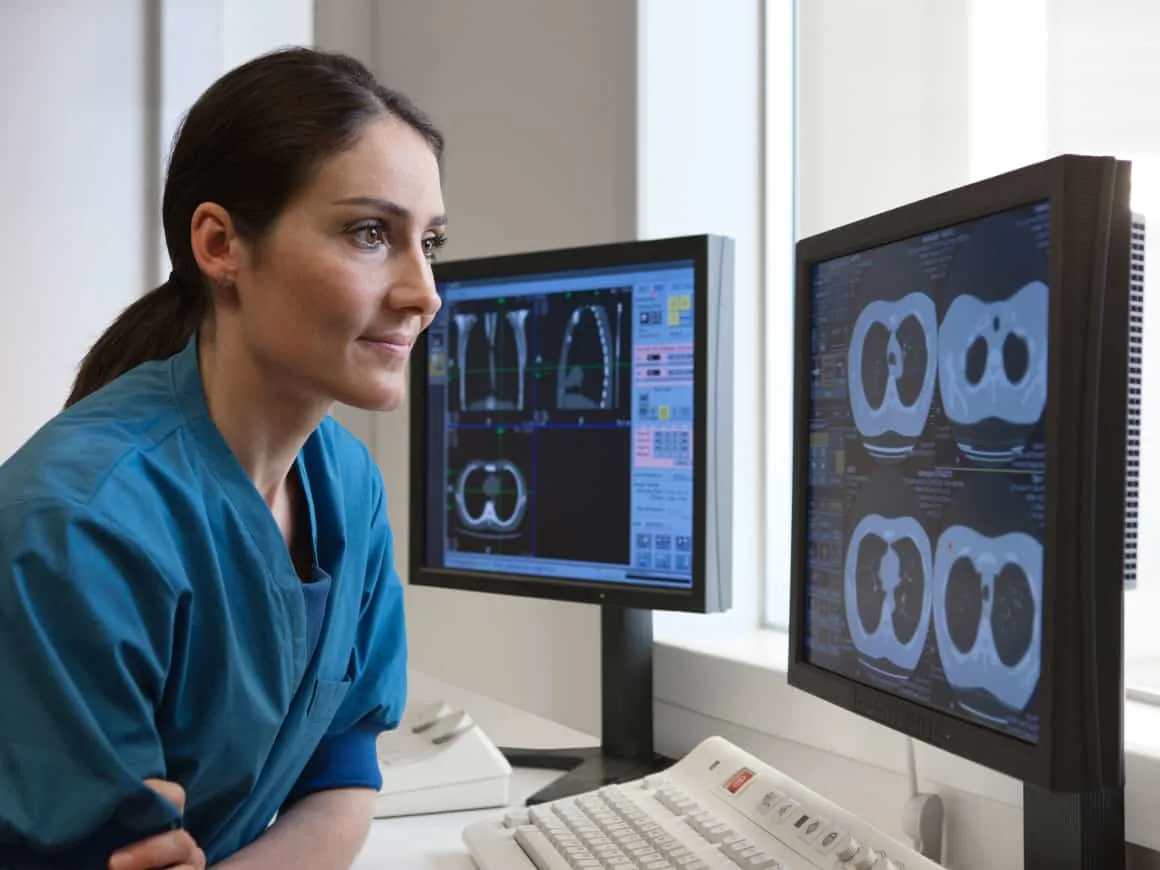
Because you want to find a better way to help your patients
Evidence-based, oncology decision support and analytics for cancer care
Integrated drug database and clinical support engine
Improve medication decisions with trusted knowledge
Evidence-based knowledge supports optimal patient care
Clinical skills for competency management and nursing procedures
