Quick Facts
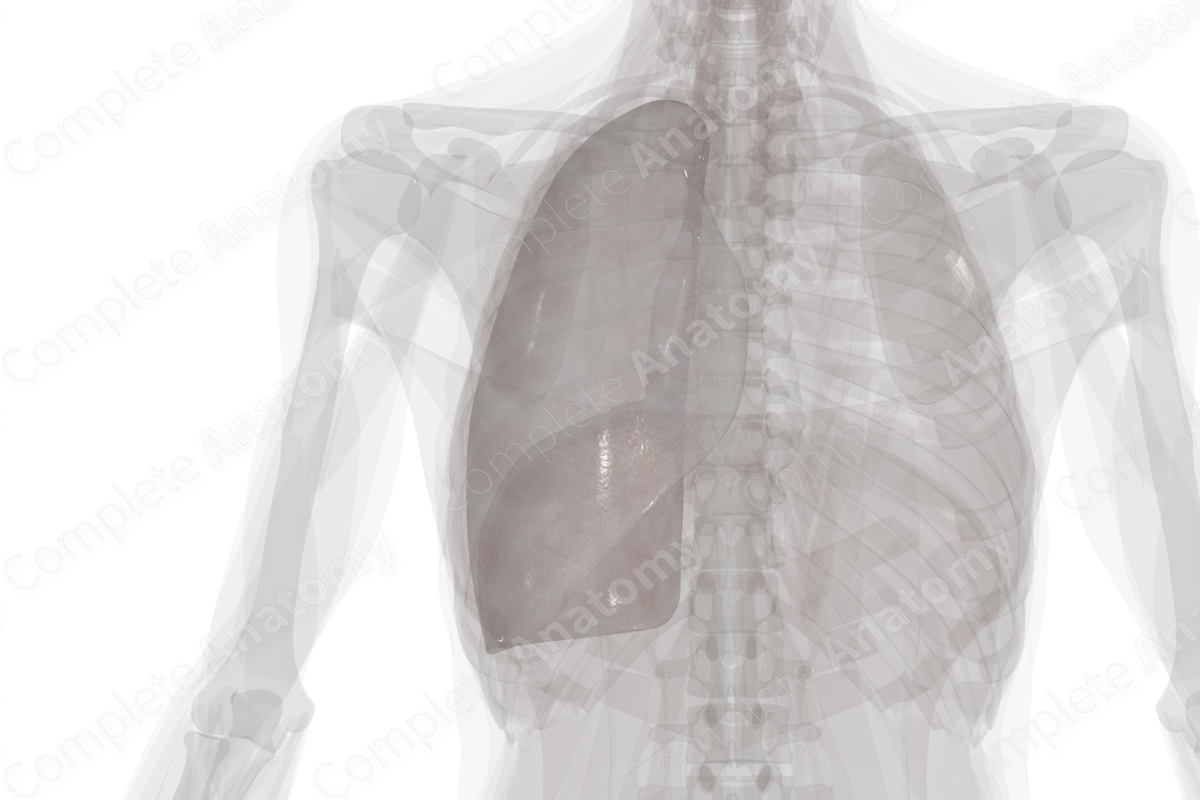
Location: Forms the external surface of the pleural cavity covering the right lung.
Arterial Supply: Internal thoracic and intercostal arteries.
Venous Drainage: Azygos system.
Innervation: anterior rami of thoracic nerves (or intercostal nerves) and branches of the phrenic nerve
Lymphatic Drainage: Superior diaphragmatic, parasternal, intercostal, and mediastinal lymph nodes.
Structure
The parietal pleura of the right lung is the outer pleural layer and lines the internal surface of the right side of the thoracic wall, the superior surface of the right hemidiaphragm, and right lateral surface of the mediastinum. It is continuous with the visceral pleura at the hilum of the right lung.
Anatomical Relations
The parietal pleura is divided into four portions; cervical, costal, diaphragmatic, and mediastinal pleurae.
- The costal parietal pleura follows the curvature of the ribs from anterior to posterior and is separated from the thoracic cage and intercostal muscles by the endothoracic fascia.
- The diaphragmatic parietal pleura lines the diaphragm inferiorly and is separated from it by the phrenicopleural fascia. This fascia is thinner and more elastic than the endothoracic fascia.
- The cervical parietal pleura lines the supraclavicular portion of the lungs and covers the apex of the lung. It is sometimes called the pleural cupula. There is a fibrous extension of endothoracic fascia which covers the cervical parietal pleura called the suprapleural membrane.
- The mediastinal pleura covers the mediastinal aspect of the lungs. There are bilateral differences between the left and the right sides due to the asymmetry of the mediastinal structures (Moore, Dalley and Agur, 2013).
The directional changes in the pleural lines are called the pleural reflections. These are the sternal, costodiaphragmatic, and vertebral reflections.
- The sternal line is the junction between the costal and mediastinal pleural regions anteriorly. There are bilateral differences between the sternal lines on the left and right sides due to the position of the heart.
- The line of reflection between the costal and diaphragmatic regions of parietal pleura is called the costodiaphragmatic line.
- The vertebral line of reflection is more gradual and sits at the junction between costal and mediastinal pleural posteriorly. It runs parallel to the vertebral column from T1—T12.
The pleural cavity is larger than the lungs. Its continuation inferiorly, beyond the lung, is called the costodiaphragmatic recess. An additional recess, called the costomediastinal recess, sits between the posterior aspects of the sternum and the costal cartilages.
Function
Within the pleural cavity, a thin layer of fluid is produced by the serous epithelial membrane lining the visceral and parietal pleurae. In addition, the visceral pleura invests all surfaces of the lung and gives the lung a shiny appearance. This smooth surface and fluid layer allow friction-free movement during respiration. Additionally, the fluid in the pleural cavity provides surface tension, akin to water between two pieces of glass, that keeps the lung surface in contact with the thoracic wall (Moore, Dalley and Agur, 2013). This permits the parietal pleura to adhere to the inner thoracic wall, the diaphragm, and the mediastinum, and thus, keep the lungs inflated. The costodiaphragmatic and costomediastinal recesses form additional spaces that permit lung expansion during forced inspiration.
Arterial Supply
The parietal pleural receives its arterial supplied according to its position within the thoracic cavity. The costal pleura receives vascular supply from the arteries that supply the thoracic wall, including the intercostal and internal thoracic arteries. The mediastinal pleura is supplied via bronchial vessels. The diaphragmatic pleura receives its supply from the vessels supplying the diaphragm, while the cervical pleura is supplied by branches of the subclavian artery.
Venous Drainage
Venous drainage of the parietal pleura occurs via thoracic wall veins which drain into the azygos system.
Innervation
The parietal pleura is innervated according to its position within the thoracic cavity. The costal and diaphragmatic parietal pleurae are innervated by the intercostal nerves (or anterior rami of the thoracic nerves) and pain is associated with the corresponding portion of the thoracic or abdominal wall. The mediastinal and central diaphragmatic parietal pleura are innervated by the phrenic nerves and pain may be referred to the tip of the shoulder i.e., dermatomes C3-C4 (Standring, 2016).
Lymphatic Drainage
Lymph from the parietal pleura drains into the superior diaphragmatic, parasternal, intercostal, and mediastinal lymph nodes.
List of Clinical Correlates
- Pneumothorax
- Hydrothorax
- Hemothorax
- Chylothorax
- Pleurectomy
- Pleurisy
References
Moore, K. L., Dalley, A. F. and Agur, A. M. R. (2013) Clinically Oriented Anatomy. Clinically Oriented Anatomy 7th edn.: Wolters Kluwer Health/Lippincott Williams & Wilkins.Standring, S. (2016) Gray's Anatomy: The Anatomical Basis of Clinical Practice. Gray's Anatomy Series 41 edn.: Elsevier Limited.
Learn more about this topic from other Elsevier products